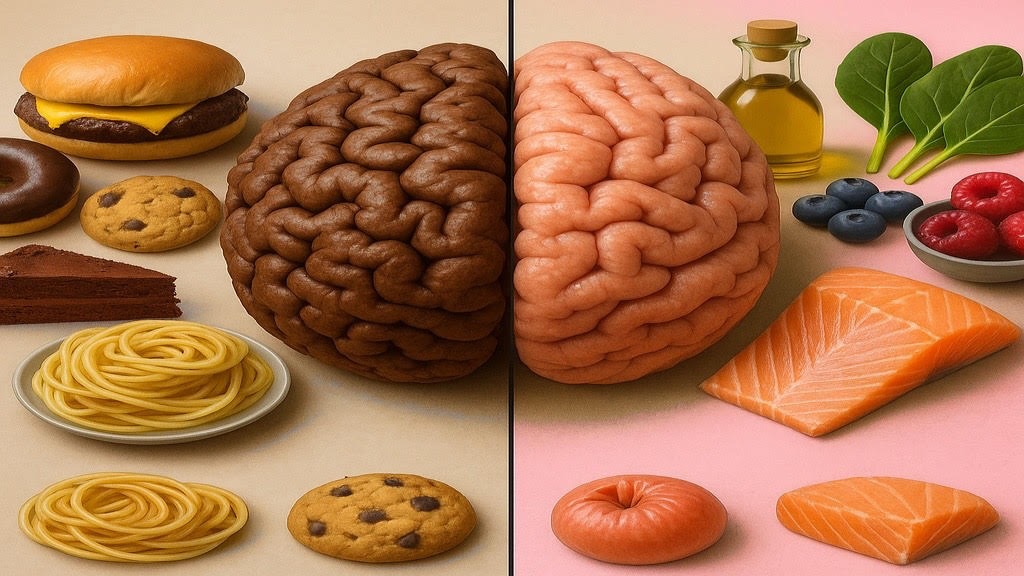
As the global population ages, the rate of dementia continues to rise — with Alzheimer’s disease leading the charge as the most common form. But here’s what many don’t realize: while there’s currently no cure for Alzheimer’s, there is a powerful way to reduce the risk and slow its progression. It starts with understanding what Alzheimer’s is — and taking action through lifestyle, exercise, and diet.
What Is Dementia and Alzheimer’s Disease?
Dementia is a broad term for a decline in cognitive function that interferes with daily life. It includes various types such as:
Vascular dementia – caused by impaired blood flow to the brain
Frontotemporal dementia – a group of disorders related to abnormal brain structure
Alzheimer’s disease – a neurodegenerative disorder and the most prevalent cause of dementia
The Hallmarks of Alzheimer’s
Alzheimer’s is driven by two primary pathologies in the brain:
β-amyloid plaque buildup
Neurofibrillary tangles of a protein called tau
These changes disrupt communication between neurons and eventually lead to brain cell death. In recent years, researchers have also focused on neuroinflammation — chronic inflammation in the brain — as a contributing factor.
Alzheimer’s is diagnosed through a combination of clinical symptoms, cognitive testing, and advanced imaging or biomarker analysis. While treatments exist to manage symptoms, no cure has yet been found.
The SHIELD Model: A Lifestyle-Based Prevention Strategy
Harvard neurologist Dr. Rudolph Tanzi helped develop the SHIELD model, a science-backed approach to preserving brain health based on epidemiological data. SHIELD isn’t a cure, but it offers real hope for prevention and slowing decline.
S – Sleep:
Deep, restorative sleep helps the brain detox — literally. During sleep, the brain clears out harmful waste proteins like amyloid. Aim for 7–8 hours nightly or take short restorative naps.H – Handle Stress:
Chronic stress is a major brain-aging factor. Activities like meditation, journaling, or engaging in fun, creative tasks help shift the brain from survival mode to thrive mode.
I – Interact:
Social isolation is a significant risk factor for dementia. Strong social ties and emotional connection are as crucial for your brain as nutrition and exercise.
E – Exercise:
What’s good for the heart is good for the brain. Exercise increases blood flow, reduces inflammation, supports the growth of new brain cells, and helps regulate insulin — all critical for long-term cognitive health.
L – Learn New Things:
Mental stimulation builds cognitive reserve — essentially a “savings account” of brain power. The more synapses you create through learning, the better your brain can resist decline.
D – Diet:
A diet that reduces inflammation, supports the gut microbiome, and stabilizes blood sugar is foundational for brain health.
Nutrition: Fuel for a Healthy Brain
The connection between the gut and brain — known as the gut-brain axis — is now undeniable. The vagus nerve, a major communication pathway between the gut and brain, is influenced by gut bacteria. These microbes can modulate memory and mood, making nutrition a key player in cognitive health.
What to Avoid
1. The Western Diet:
High in processed foods, sugars, and unhealthy fats, this diet increases inflammation, disrupts the gut microbiome, and accelerates cognitive decline.
2. Refined Sugars:
Excess sugar feeds bad gut bacteria, spikes insulin, and promotes brain inflammation.
3. Gluten (for sensitive individuals):
For those with celiac disease or gluten sensitivity, gluten may worsen brain fog and cognitive decline.
What to Eat for a Sharp Mind
🍇 Berries:
Rich in antioxidants and fiber, berries fight oxidative stress and support gut health.
🥬 Leafy Greens:
Packed with folate and other essential nutrients, greens like spinach and Swiss chard help protect brain function.
🐟 Omega-3s:
Found in wild-caught fish, flaxseeds, and walnuts, omega-3 fats reduce inflammation and support neuronal health.
🫒 Extra Virgin Olive Oil:
Promotes autophagy — the brain’s internal cleaning system — and is linked to lower Alzheimer’s rates.
🧄 Spices:
Turmeric (with black pepper), cinnamon, saffron, and rosemary have potent anti-inflammatory and mood-boosting properties.
🥗 The MIND Diet:
A fusion of the Mediterranean and DASH diets, the MIND Diet emphasizes whole, nutrient-dense foods that reduce Alzheimer’s risk and slow cognitive decline.
Exercise: Move It to Save It
Regular movement improves mood, memory, and metabolism. Cardiovascular exercise, strength training, and even yoga all improve brain blood flow, decrease inflammation, and support neurogenesis — the creation of new neurons.
Aim for:
150 minutes of moderate activity weekly
2–3 strength sessions/week
Daily movement breaks to counter sedentary behavior
Final Thoughts: Build a Brain-Healthy Lifestyle
Alzheimer’s disease is a complex, multifactorial condition — but the way we live can change the story. With sleep, connection, learning, movement, stress management, and a powerful, gut-supportive diet, we can build real resilience in the brain.
“The mind is just like a muscle — the more you exercise it, the stronger it gets and the more it can expand.” — Idowu Koyenikan
Let’s treat every day as a chance to train our brains, nourish our bodies, and strengthen our futures.











Write A Comment